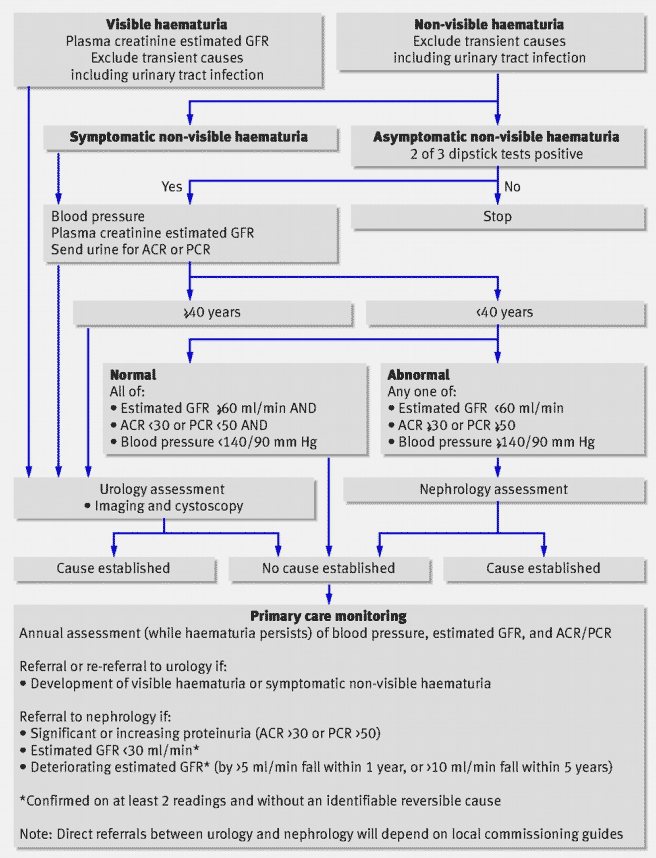
Non-visible Haematuria
Condition: Non-visible Haematuria
Section Author: Jon Rees
Review Date: September 2017
Overview
Another controversial issue – the management of non-visible haematuria (NVH) in primary care.
Non-visible haematuria is now the recommended terminology, replacing phrases such as ‘dipstick haematuria’ and ‘microscopic haematuria’.
Some key issues for primary care:
- When to test for haematuria – screening is not recommended, and much of the difficulty in managing this finding can be avoided if urine is tested for blood only in appropriate circumstances.
- When to refer patients with NVH to secondary care for further investigation – not all patients with NVH need urological or nephrological assessment – patients with asymptomatic NVH found below the age of 40, with normal renal function, can be managed in primary care – the BAUS / Renal Association guidelines have full detail of this.
- When to refer patients with NVH via the 2 week wait suspected cancer pathway – this was updated in 2015 in the NICE Referral for Suspected Cancer Guidelines. Remember though that if patients do not meet the 2 week wait criteria, they may still need referral outside of this pathway, according to the BAUS / Renal Association guidelines, which still apply. NICE guidelines should only be used to determine the urgency of referral.
Summary of NICE guidance (all haematuria ie including Visible Haematuria), June 2015:
Remember that the criteria below ONLY tell you who to refer urgently via a two week wait pathway – many patients who do not meet these criteria will need an urgent urological referral for further investigation.
Healthcare Professional Links
Guidelines for management of non-visible haematuria in primary care – produced by British Association of Urological Surgeons and the Renal Association in 2009, and still the key document to understand: ‘Assessment and management of non-visible haematuria in primary care’. Kelly JD et al. BMJ 2009; 338: a3021. http://www.bmj.com/content/338/bmj.a3021
Haematuria – 10 Top Tips for Primary Care, published by MacMillan Cancer Support 2016: http://www.macmillan.org.uk/documents/aboutus/health_professionals/primarycare/10toptips/primary-care-ten-tips-haematuria.pdf
NICE guideline (NG12): Suspected cancer: recognition and referral. June 2015. https://www.nice.org.uk/guidance/ng12
‘Blood in Pee’ campaign – information from Cancer Research UK: http://www.cancerresearchuk.org/health-professional/early-diagnosis-activities/be-clear-on-cancer/blood-in-pee-campaign/information-for-gps-and-other-healthcare-professionals#ordercampaignmaterials
‘Blood in Pee’ campaign – information for patients on NHS Choices: https://www.nhs.uk/be-clear-on-cancer/symptoms/blood-in-pee#IGuglv5yUoT2V28U.97
Kelly JD et al. BMJ 2009; 338: a3021
Information for patients
BAUS http://www.baus.org.uk/patients/conditions/2/blood_in_the_urine_haematuria
Renal Association http://www.renal.org/information-resources/the-uk-eckd-guide/haematuria